Iliotibial band syndrome is inflammation and pain on the the outer side of the knee. The iliotibial band is a layer of connective tissue. It begins at a muscle near the outside of the hip, travels down the outer side of the thigh, crosses the outside of the knee and attaches to the outer side of the upper tibia.
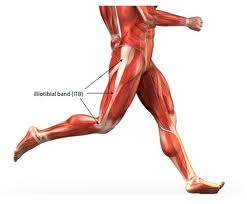 Iliotibial band syndrome occurs when this band repeatedly rubs over the condyle of the femur, causing the band to become irritated. Many times this is due to jogging or running.
Iliotibial band syndrome occurs when this band repeatedly rubs over the condyle of the femur, causing the band to become irritated. Many times this is due to jogging or running.
The condition can result from tight muscles, connective tissue, discrepancy in leg length, and running on sloped surfaces.
Iliotibial Band Syndrome: Diagnosis/Definition
The iliotibial band (ITB) is a thick band of connective tissue that runs along the outside of the thigh. Iliotibial band syndrome is an overuse injury caused by repetitive friction of the ITB across the knee joint area.
Iliotibial Band Syndrome: Initial Diagnosis and Management
- History and physical examination
- Relative rest: decrease or stop running
- Ice and massage
- NSAIDs
- Adults – 200 to 400 milligrams (mg) every four to six hours as needed for up to 2 weeks. Example: Ibuprofen
- Take tablet or capsule forms of these medicines with a full glass (8 ounces) of water.
- Do not lie down for about 15 to 30 minutes after taking the medicine. This helps to prevent irritation that may lead to trouble in swallowing.
- To lessen stomach upset, these medicines should be taken with food or an antacid.
- Stretches and strengthening
- Appropriate restrictions of activity
Iliotibial Band Syndrome: Ongoing Management and Objectives
- Rest is individualized depending upon severity
- Ice for 10 to 15 minutes with hourly reapplication.
- Slow and sustained active stretches
Iliotibial Band Syndrome: Indication a Profile is Needed
- Any limitations that affect strength, range of movement, and efficiency of feet, legs, lower back and pelvic girdle.
- Slightly limited mobility of joints, muscular weakness, or other musculo-skeletal defects that may prevent moderate marching, climbing, timed walking, or prolonged effect.
- Defects or impairments that require significant restriction of use.
